The aetiology of multiple sclerosis (MS) has remained unclear, but a causative contribution of factors outside the central nervous system (CNS) is conceivable. It was recently suggested that gut bacteria trigger the activation of CNS-reactive T cells and the development of demyelinative disease.
METHODS: C57BL/6 (B6) mice were kept either under specific pathogen free or conventional housing conditions, immunized with the myelin basic protein (MBP)-proteolipid protein (PLP) fusion protein MP4 and the development of EAE was clinically monitored. The germinal center size of the Peyer's patches was determined by immunohistochemistry in addition to the level of total IgG secretion which was assessed. MP4-specific T cell and B cell responses in the Peyer's patches and the spleen were measured. Ear swelling assays were performed to determine the extent of delayed-type hypersensitivity reactions in specific pathogen free and conventionally housed mice.
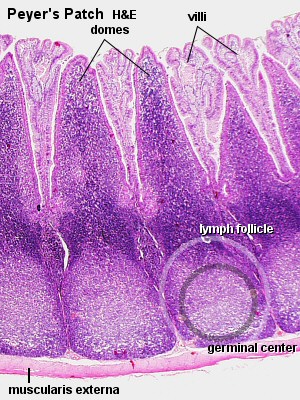
RESULTS:In B6 mice that were actively immunized with MP4 and kept under conventional housing conditions clinical disease was significantly attenuated compared to specific pathogen free mice. Conventionally housed mice displayed increased levels of IgG secretion in the Peyer's patches (a lymph gland in the gut) , while the germinal center formation in the gut and the MP4-specific TH17 response in the spleen were diminished after immunization. Accordingly, these mice displayed an attenuated delayed type hypersensitivity (DTH) reaction in ear swelling assays.
CONCLUSIONS: The data corroborate the notion that housing conditions play a substantial role in the induction of mouse EAE and suggest that the presence of gut bacteria might be associated with a decreased immune response to antigens of lower affinity. This concept could be of importance for MS and calls for caution when considering the therapeutic approach to treat patients with antibiotics.
This is yet another post that implicates gut microbes as being important in the control of the immune response. Specific pathogen free means that the animals do not have a long list of harmful pathogens and they are often kept in isolators to protect this status. In a conventional housing state the animals are kept in open cages. It does not mean however they will be exposed to more real pathogens than in the pathogen-free conditions, however the gut microbes may end up being different. In this study "dirty" animals in conventional cages got less disease and so they suggest that antibiotics may be dangerous. However there are many cases where an antibiotic has been given to mice and it has made their disease better. Likewise it is well accepted that infections can trigger relapses. If you are on antibiotics make sure you use them correctly and only use them where necessary as in appropriate use is leading to anti-biotic resistance.
However will this fuel the opening of more Feacal transplant resorts?